Bio-printing skin to heal chronic wounds
A printing technique that simulates all three layers of the human skin could potentially repair deep and difficult-to-repair chronic wounds.
Often the top of an injury heals before the bottom, so the wound collapses in on itself – over time, this can lead to scar tissue and reduced skin function.
Scientists from the Universities of Birmingham and Huddersfield, UK, have deployed suspended layer additive manufacturing (SLAM) to print skin equivalents using bio-inks.
Human skin comprises three layers – the hypodermis, or fatty layer; the dermis; and the epidermis. Although a number of skin replacements exist, so far it has not been possible to replicate the compositional, mechanical and cellular structure of human skin.
Alan Smith, Professor of Biopolymer Science at Huddersfield University and co-author of a paper published in the research journal APL Bioengineering, notes, ‘You have three different cell types [and] they all grow at different speeds. If you try to produce tri-layered structures, it can be very difficult to provide each of the requirements of each different layer.’
However, Jess Senior, a PhD student at Huddersfield, used the SLAM technique to develop a continuous tri-layered structure that repeats the distinct tissue environments in the hypodermis, dermis and epidermis.
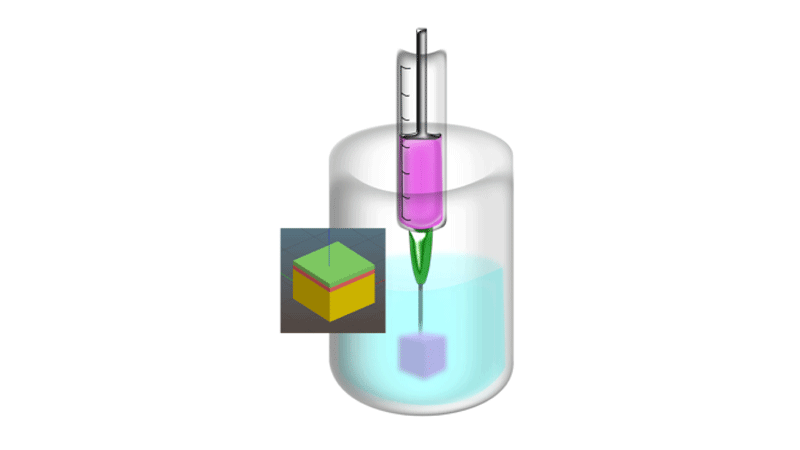
Computer aided design has been used to develop the construct, which is printed using bio-inks of pectin blended with collagen.
‘Senior was able to tailor the stiffness and create a structure that could support each of the cell types required,’ explains co-author Liam Grover, Professor in Biomaterials Science at the University of Birmingham.
By modifying an embedded printing approach, known as Freeform Reversible Embedding of Suspended Hydrogels (FRESH), the scientists have also created a supporting bed to solidify the three layers. This gel-like material twists and alters its structure as it forms to create a bed of particles that can then support a second phase of gel injection.
‘Rather than being formed from broken up gel particles, our materials are formed by the application of a gentle shear during gelation,’ explains Grover.
‘The resulting particles are dispersed in an uncrosslinked polymer. When they come into contact with each other, they rapidly form a gel-like material, which can then be broken up by shear. When the shear is removed, they once again harden. In comparison with other suspended methods, the supporting bed we have made heals more rapidly and this should theoretically improve resolution.’
During printing, the skin layers are deposited in the supporting gel, which holds the different layers in place. After printing, it is washed away, leaving behind the layered skin equivalent.
To help mimic skin composition, the researchers have blended different ratios of collagen and pectin. As the research paper explains, ‘the use of a relatively high proportion of pectin enabled the confinement of adipose derived mesenchymal stem cells’, which are well known for their role in repair and regeneration.
To test the skin substitute, the team has cut a hole in pig tissue using a scalpel, printed a skin equivalent to fill the hole and cultured the model for 14 days.
‘We used a stain that allowed us to quantify the integration we got between the original material and tissue,’ adds Grover. ‘We were able to demonstrate some integration even after a short period of time.’
However, the modelling does have its limitations for assessing chronic wound healing. ‘To allow us to move the technology forwards, we will have to show that it can be used to support proper tissue healing in an animal chronic wound model,’ continues Grover. ‘Once we have shown this, we can start to consider moving towards human trials.’

